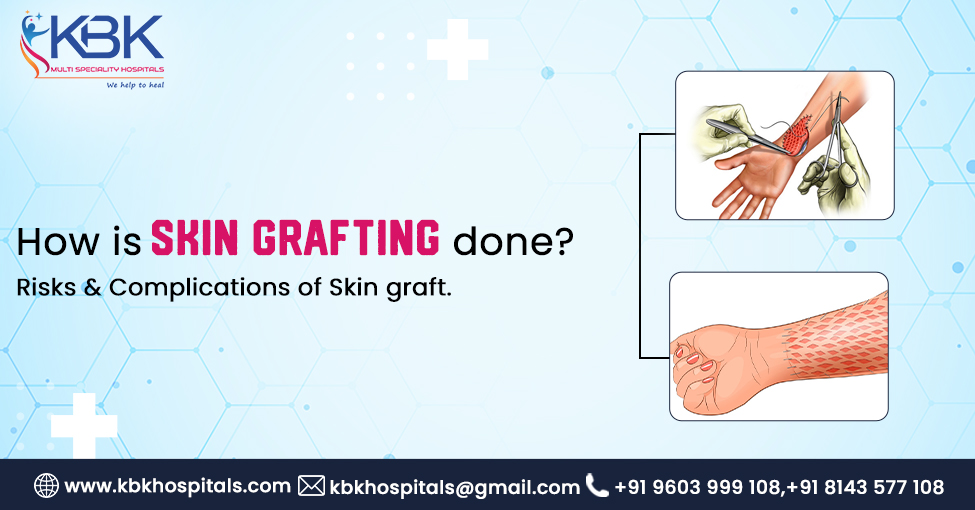
Introduction
Skin grafting is a medical procedure or surgery to restore your real skin. It involves removing skin from one body area and transplanting it to cover where tissue has been lost due to injury or surgery. People use skin grafting for many reasons. Such as restoring loss of physical function and appearance by using transplanted healthy skin, repairing scars or skin defects caused by burn injuries, and resurfacing hands and feet that have suffered significant tissue loss due to tendon repairs. There are different types of skin grafts, each offering advantages and potential risks and complications.
What is a skin graft?
Skin grafting is a remarkable surgical technique where healthy skin embarks on a journey from one part of your body to another, heroically rescuing damaged or missing skin. This noble graft forms blood vessels within days and becomes one with its new surroundings.
Skin graft surgery comes to the rescue for individuals with skin damage due to burns, injuries, diseases, or infections. Skin graft surgery is a good choice for those who’ve undergone skin cancer removal. The recovery skin graft healing time post-surgery varies based on factors like personal health, graft size, and the technique implemented by the medical expert. With a high success rate, most skin graft procedures work effectively on their first attempt. However, if the transplanted skin doesn’t heal well, a subsequent skin graft recovery might be needed to ensure seamless integration.
What are the sources of healthy skin for grafts?
Autografts reign supreme through the skin graft process, where healthy skin from one’s body is skillfully transferred to an area in need. Occasionally, a person may lack good healthy skin, leading to an intriguing search for alternatives, and then the cadaver skin bravely steps in as a solution. This process is called skin allograft.
In some cases, for a temporary fix, the skin grafting procedure is also complete with animal skin, like pig skin. This process is called a xenograft. Both skin allografts and xenografts gallantly shield the damaged skin, paving the way for wound healing or the emergence of new healthy skin for a permanent graft.
Types of skin grafts:
Many types of skin grafting are there. But the most popular are split-thickness grafts and full-thickness grafts.
1. Split-thickness Skin grafts :
This split-thickness skin graft recovery procedure involves carefully extracting the epidermis, which is the skin’s top layer, along with a portion of the deeper layer called the dermis, from a healthy area in the body. Often found on the front or outer thigh, abdomen, buttocks, or back, the skilled surgeon removes the skin layers necessary to fix the damaged skin.
A surgeon can cover more damaged skin areas using this powerful procedure. Though fragile and shimmering with a shiny or smooth appearance, the resulting grafts merge seamlessly yet may exhibit a paler hue than the surrounding skin.
It’s important to remember that these grafts, like a tender sapling, may not grow as swiftly as ungrafted skin. Hence, children who receive them may require additional grafts as their bodies flourish into adulthood.
2. Full-thickness Skin grafts:
The full-thickness graft procedure is a little complicated if it is on a visible part. In this procedure, the surgeons delicately do every process to fix the skin. It removes both the epidermis and dermis from a hidden corner of your body, like the abdomen, groin, forearm, or just above your collarbone.
These small skin fragments are then meticulously sutured or stapled to cover small, highly visible wounds, especially on the face. The magic of full-thickness grafts lies in their seamless blending with the surrounding skin, resulting in a more aesthetically pleasing outcome than their split-thickness counterparts.
3. Composite graft:
This composite graft is suitable for soft skin. This procedure involves a skin transplant. Through this composite grafting process, you can repair soft skin like the nose, ears, fingertips, etc.
How does a skin graft help?
The skin graft is required when your skin suffers some serious damage. This medical marvel steps in when your body can’t regenerate the skin. These grafts help to recover from many conditions, such as intense burns, serious post-surgical skin removal, stubborn ulcers or bedsores, and extra-large, slow-healing wounds. Life’s bumps and bruises don’t stand a chance with skin grafts!
Skin graft procedure :
The skilled surgeon starts the skin graft procedure by carefully removing skin from the hidden depths of the donor site. If the patient needs a split-thickness graft, the surgeon might choose mysterious places like the hip or the outside of the thigh, which clothes can cover.
But if a full-thickness graft is in order, the surgeon will choose to uncover the secrets of your abdomen, groin, forearm, or the area above the collarbone. Using surgical dressing, staples, or stitches, the surgeon will secure the skin onto the transplant area after getting it from the donor site.
Finally, the surgeon thoughtfully applies a non-stick dressing to the donor site for some days.
A vibrant purple or scarlet hue adorns the skin within the initial days. As time dances along, the doctor’s skilled unveiling, roughly a week later, reveals a blush-toned surface. Patience pays off as the skin eventually harmonizes with its neighbors, seamlessly blending in.
Aftercare process for skin graft :
The patient must stay at the hospital for some days if it is a split-thickness skin graft. Their staff monitors each sign, then suggests medications for pain. After 7 days, the grafted skin will connect with the surrounding skin and develop blood vessels. If this process does not begin in 10 days, it is a negative sign. Maybe the body can’t accept the graft. Infections, too much movement, and poor blood flow are reasons for not accepting body skin.
To recover from that, the doctor may suggest another surgery. To keep your dressing safe, you must clean and dry your bandage. Don’t make more movement to the grafting area. Sitting or lying down, elevate the graft location above the surface of the heart to help lessen swelling and fluid retention.
Your doctor will remove the bandage after a few days, and you must refrain from picking, scratching, or contacting the skin transplant.
Caring for the Skin graft donor site healing :
The aftercare process is one of your crucial missions to safeguard the Skin graft donor site healing. There is a thin bandage that will shield the area from unwanted contact.
Brace yourself for a few days of sensations: the sting of victory and a touch of liquid oozing from your hardy donor site. Call your doctor for backup if you encounter intense villainous pain or swelling.
The skin graft donor site will take 7 to 10 days to heal. After removal of the bandage, you can see a pink surface of your skin. The original color will slowly re-emerge in due time.
Conclusion
Skin graft surgery is an effective technique for treating injured areas of the skin. Skin transplant is often a preferred treatment over more invasive procedures. Although the procedure carries some risks and complications, such as infection, scarring, blood clots, and vascular compromise, pain-free therapy can usually minimize these. Visit KBK Multispeciality hospital to learn more about how skin grafting and the healing after surgery can help you achieve your desired outcome safely. Depending on the type of graft used and its location on the body, recovery times can range from 10 days to 1 month.
FAQs:
1. Can skin graft scars be removed?
The complete removal of skin graft scars may not always be possible. Various methods are available to help minimize their appearance is reassuring. Dermatologists and plastic surgeons continuously develop techniques to improve skin graft scars. Such as laser therapy, dermabrasion, and silicone gel applications. In some situations, additional surgery may be performed to reduce the scar’s size, improve its shape, or correct irregular pigmentation. The success of these treatments depends on the severity of the scar, age, and individual skin characteristics.
2. Are skin grafts painful?
Undergoing a skin graft can elicit fear and apprehension, especially when considering the potential pain. The procedure is performed under anesthesia to ensure the patient experiences no pain. During the post-operative recovery, some discomfort and pain may arise. Factors such as incision site sensitivity, donor site pain, and potential complications such as infection may contribute to the discomfort felt by the patient.
3. When skin graft is necessary?
If the body’s natural ability to heal is insufficient, skin grafts become necessary. It is generally required in cases where large areas of skin are lost due to burns, infections, serious injuries, or surgical procedures. Skin grafts may be essential in treating chronic wounds, such as ulcers, and reconstructing defects resulting from skin cancer removal.
4. Does skin grafting leave scars?
The healing potential of skin grafting is certainly impressive. But if the case is severe, it leaves noticeable scars. The visibility and extent of scarring can vary greatly depending on factors such as the individual’s skin type, age, and graft size. The scar treatments and aftercare recommendations can greatly improve scar appearance and overall outcomes.
5. Can skin grafts get infected?
The grafting process involves taking skin from a donor site and transplanting it onto the wound site. Sometimes the body’s immune response might counteract the healing process. This can result in inflammation, redness, and pus discharge in severe cases. Additionally, since the newly grafted skin can be more delicate, there is an increased vulnerability to bacterial infection. Despite advances in medical technology and hygiene protocols, the possibility of infection still exists.